Comprehensive guidelines, like those from 2013 and 2014, emphasize a multi-modal approach, integrating medication, injections, and crucially, targeted physical therapy interventions.
What is Complex Regional Pain Syndrome (CRPS)?
Complex Regional Pain Syndrome (CRPS) is a chronic pain condition typically affecting an arm or a leg, though it can occur in other body parts. Often, CRPS develops after an injury, surgery, stroke, or heart attack, but sometimes the trigger isn’t identifiable. The pain experienced is disproportionate to the severity of the initial injury, and it’s characterized by a constellation of symptoms beyond just pain.
These symptoms can include changes in skin color and temperature, swelling, altered sweating patterns, and sensitivity to touch. Over time, CRPS can lead to decreased range of motion, muscle weakness, and even functional limitations impacting daily activities. Understanding the evolving perspectives on CRPS, as highlighted in review articles from 2014 and later, is crucial for effective management. Early intervention, including a carefully structured physical therapy protocol, is paramount in mitigating the progression of this debilitating condition and improving patient outcomes.
The Role of Physical Therapy in CRPS Management
Physical therapy and rehabilitation are fundamental components of CRPS management, as consistently emphasized in practical diagnostic and treatment guidelines since 2012. It’s not simply about ‘exercise’; it’s a carefully graded, phased approach designed to address the multifaceted nature of the syndrome. Interventions aim to restore function, reduce pain, and prevent further disability.
Techniques range from gentle range of motion exercises in the acute phase to more robust functional restoration training in the chronic stages. Crucially, approaches like mirror therapy, documented in Scandinavian Journal of Pain research (2024), and Graded Motor Imagery (GMI) play a vital role in re-training the nervous system. The goal is to modulate pain signals, improve sensory processing, and ultimately, empower patients to regain control over their lives. A well-defined protocol, tailored to the individual’s phase of CRPS, is essential for optimal results.

Diagnostic Criteria & Assessment
Accurate diagnosis relies on clinical criteria, as outlined in guidelines from 2013, alongside thorough assessment to understand individual symptom presentation and guide therapy.
Budapest Criteria for CRPS Diagnosis
The Budapest Criteria represent a significant advancement in standardizing the diagnosis of Complex Regional Pain Syndrome (CRPS). Developed to address limitations of earlier diagnostic approaches, these criteria emphasize a scoring system based on a combination of sensory, motor, autonomic, and swelling-related symptoms. The criteria categorize patients into probable, complete, and incomplete CRPS based on the accumulated score.
Sensory symptoms include continuous pain disproportionate to the inciting event, allodynia (pain from non-painful stimuli), and hyperalgesia (increased pain from painful stimuli). Motor symptoms involve weakness, tremor, or dystonia. Autonomic dysfunction manifests as temperature, skin color, or sweating abnormalities. Swelling is also a key component.
Utilizing these criteria is crucial for initiating appropriate treatment, including a tailored physical therapy protocol. A precise diagnosis, guided by the Budapest Criteria, ensures that interventions are focused and effective in managing the multifaceted symptoms of CRPS, ultimately improving patient outcomes and quality of life.
Physical Assessment Techniques for CRPS
A thorough physical assessment is paramount in characterizing the unique presentation of CRPS in each patient, informing a targeted physical therapy protocol. This begins with a detailed history, exploring the onset, progression, and characteristics of pain. Objective measures include assessing range of motion, strength, and reflexes, noting any asymmetries.
Crucially, evaluating sensory function is vital – testing for allodynia and hyperalgesia using light touch, pinprick, and thermal stimuli. Assessing autonomic function involves observing skin temperature, color changes, and sweat patterns. Edema measurements and vascular assessments are also essential.
Furthermore, specialized tests like two-point discrimination and temporal summation can reveal subtle sensory deficits. Documenting these findings provides a baseline for tracking progress and adjusting the physical therapy intervention strategy, ensuring it remains responsive to the patient’s evolving needs.

Phase 1: Acute Phase Physical Therapy Protocol
Initial interventions focus on pain and edema control, utilizing gentle movements, splinting, and vitamin B supplementation, alongside pharmacological management strategies.
Goals of Acute Phase Therapy
The primary objectives during the acute phase of Complex Regional Pain Syndrome (CRPS) physical therapy are centered around mitigating pain, reducing inflammation, and preventing further functional decline. A crucial goal is to protect the affected limb, often achieved through splinting, to minimize irritation and encourage a pain-free environment.
Early intervention aims to control edema, a common symptom, utilizing elevation and gentle techniques. Maintaining a degree of range of motion is vital, even if limited, to prevent joint stiffness and contractures, but this must be carefully balanced with pain levels.
Psychological support is also a key component, addressing the anxiety and fear often associated with CRPS. The overarching aim isn’t aggressive rehabilitation at this stage, but rather symptom management and laying the groundwork for subsequent phases of therapy. Preventing maladaptive pain behaviors is also paramount, preparing the patient for a more active role in recovery.
Gentle Range of Motion Exercises
During the acute phase, range of motion (ROM) exercises must be exceptionally gentle and pain-guided. The focus isn’t on achieving full ROM, but on preventing joint stiffness and maintaining a minimal level of movement without exacerbating pain. These exercises are typically passive or active-assisted, meaning the therapist or a device assists the patient’s movement.
Exercises should be performed slowly and deliberately, carefully monitoring the patient’s response. Any increase in pain, swelling, or skin color changes signals the need to immediately reduce the intensity or stop the exercise.
Simple pendulum exercises, wrist and ankle pumps, and gentle finger/toe extensions are often utilized. The goal is to encourage fluid movement and prevent the limb from becoming immobile, preparing it for more active rehabilitation as the condition stabilizes. Consistent, low-intensity movement is preferred over infrequent, aggressive attempts.
Edema Management Techniques
Edema, or swelling, is a common symptom in the acute phase of CRPS, contributing significantly to pain and limited function. Physical therapy interventions prioritize reducing this swelling to improve comfort and facilitate movement. Elevation of the affected limb above heart level is a foundational technique, promoting fluid drainage.
Gentle compression therapy, utilizing specialized bandages or sleeves, can help minimize edema formation and provide support. Manual lymphatic drainage (MLD), a specialized massage technique, encourages lymphatic flow and reduces fluid accumulation.
Precise application and monitoring are crucial; excessive compression can worsen pain. Combining these techniques with controlled movement, as in gentle ROM exercises, further enhances fluid mobilization. Patient education on self-management strategies, like intermittent elevation and proper bandaging, is essential for continued edema control.

Phase 2: Subacute Phase Physical Therapy Protocol
This phase shifts towards pain modulation and restoring function, employing desensitization, graded motor imagery, and mirror therapy to address central sensitization.
Pain Modulation Techniques
During the subacute phase, pain modulation techniques are paramount in managing CRPS symptoms. These strategies aim to reduce the amplified pain signals reaching the brain and restore a more normal sensory experience. A key component involves gentle, progressive exercises designed not to exacerbate pain, but rather to gradually increase tolerance.
Techniques like TENS (Transcutaneous Electrical Nerve Stimulation) can be utilized to provide sensory input that competes with pain signals. Furthermore, techniques focusing on diaphragmatic breathing and relaxation exercises help regulate the autonomic nervous system, often dysregulated in CRPS, reducing sympathetic overdrive.
Careful monitoring of the patient’s response is crucial; any increase in pain should prompt modification of the technique or a temporary reduction in intensity. The goal is to ‘retrain’ the nervous system, diminishing its hypersensitivity and promoting a more balanced pain perception. Pharmacological interventions, as outlined in treatment guidelines, often complement these physical therapy approaches.
Desensitization Techniques
Desensitization techniques are central to subacute CRPS management, addressing the hypersensitivity often experienced by patients. These methods systematically expose the affected limb to progressively increasing sensory stimuli, aiming to reduce the nervous system’s exaggerated response. Initial stages involve tactile desensitization, utilizing various textures – silk, cotton, sandpaper – applied gently to the skin.
The process must be carefully graded, starting with stimuli that evoke minimal discomfort and gradually increasing intensity as tolerance improves. Visual desensitization, involving exposure to images previously associated with pain, can also be incorporated.
Crucially, patient education is vital; understanding the rationale behind desensitization empowers them to actively participate in their recovery. Monitoring for signs of symptom exacerbation is essential, and adjustments to the protocol should be made accordingly. These techniques, alongside pain modulation, form a cornerstone of effective CRPS rehabilitation.
Graded Motor Imagery (GMI)
Graded Motor Imagery (GMI) is a neuroplasticity-based approach increasingly utilized in CRPS rehabilitation, particularly during the subacute phase. It’s a three-stage program designed to ‘retrain’ the brain and reduce cortical maladaptive plasticity. The initial phase, left/right discrimination, involves identifying mirrored images of body parts, enhancing cortical representation.
Next, explicit motor imagery requires patients to mentally rehearse movements without actual physical execution, activating motor pathways. Finally, implied motor imagery involves imagining a movement while simultaneously performing a different, non-painful action.
GMI aims to normalize sensory processing and reduce pain by gradually re-establishing accurate cortical maps. Careful monitoring of symptom response is crucial, and progression should be guided by patient tolerance. Combining GMI with other techniques, like mirror therapy, can optimize outcomes.
Mirror Therapy Implementation
Mirror therapy, highlighted in Scandinavian Journal of Pain literature reviews and case reports, leverages neuroplasticity to address sensorimotor dysfunction in CRPS. Implementation involves positioning a mirror vertically between the affected and unaffected limb, allowing the patient to view the unaffected limb’s reflection as if it were the affected one.
Patients then perform slow, pain-free movements with the unaffected limb, observing the ‘illusion’ of movement in the affected limb. This visual feedback can reduce pain and improve function by challenging maladaptive cortical representations.
Sessions typically last 15-30 minutes, several times a week. Careful monitoring for increased pain or distress is essential. Success relies on creating a convincing illusion and encouraging active engagement. Combining mirror therapy with GMI often yields synergistic benefits, enhancing cortical reorganization.

Phase 3: Chronic Phase Physical Therapy Protocol
Long-term management focuses on functional restoration, building strength and endurance, and refining proprioception to maximize independence and quality of life for patients.
Functional Restoration Training
Functional restoration training represents a cornerstone of the chronic CRPS physical therapy protocol, shifting the focus from solely pain management to regaining practical abilities. This phase emphasizes task-specific exercises designed to mimic real-life activities, progressively challenging the patient’s physical capabilities.
The goal isn’t simply to increase strength, but to improve the way movements are performed, addressing compensatory patterns developed during the earlier phases. Activities are carefully selected based on individual patient goals – returning to work, hobbies, or daily living tasks.
This training incorporates graded exposure to activities, starting with modified versions and gradually increasing complexity. A key element is promoting neuroplasticity, retraining the nervous system to interpret sensations accurately and efficiently. Emphasis is placed on proper body mechanics and pacing strategies to prevent flare-ups, ensuring sustainable improvements in function and participation.
Strength and Endurance Exercises
As CRPS transitions into the chronic phase, targeted strength and endurance exercises become integral to the physical therapy protocol. However, these are implemented cautiously, prioritizing pain modulation and avoiding exacerbation of symptoms. The focus shifts from gentle range of motion to rebuilding muscle strength and improving cardiovascular fitness.
Exercises are carefully graded, starting with low-intensity activities and progressively increasing resistance or duration. Isometric exercises are often introduced initially, minimizing joint movement and stress. Progressing to isotonic and then dynamic exercises follows, always within the patient’s pain tolerance.
Endurance training, such as walking or cycling, is incorporated to improve overall stamina and reduce fatigue. The aim is to enhance functional capacity, enabling patients to participate more fully in daily activities. Regular monitoring of pain levels and adjustments to the exercise program are crucial for optimal outcomes.
Proprioceptive Training
A significant component of chronic CRPS management involves restoring proprioception – the body’s awareness of its position in space. CRPS often disrupts this sense, contributing to impaired movement and increased risk of injury. Proprioceptive training aims to retrain the nervous system and improve joint stability.
Exercises typically involve balance activities, such as single-leg stance or using wobble boards, progressing in difficulty as the patient improves. Joint position sense exercises, where patients attempt to identify joint angles without visual cues, are also beneficial.
These exercises are performed slowly and deliberately, focusing on accurate movement and minimizing pain. The goal is to enhance neuromuscular control and improve coordination, ultimately leading to more efficient and pain-free movement patterns. Consistent practice and gradual progression are key to successful proprioceptive retraining.
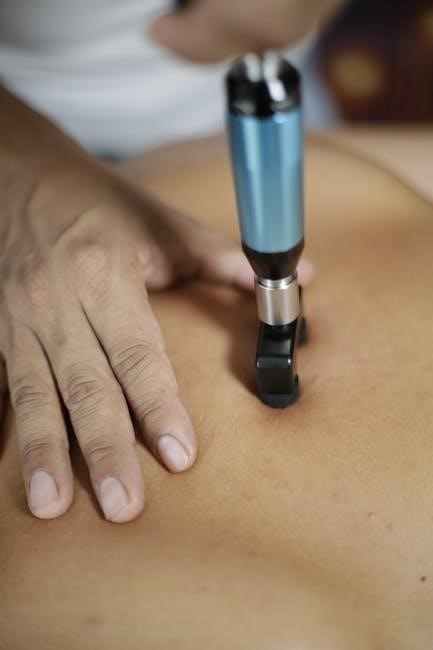
Adjunctive Therapies
Beyond physical therapy, pharmacological interventions and psychological support—including Cognitive Behavioral Therapy (CBT)—are vital for holistic CRPS management and improved outcomes.
Pharmacological Interventions (Overview)

Medication plays a significant, though not solitary, role in CRPS management, often forming a crucial component alongside physical therapy and psychological support. Treatment frequently begins with over-the-counter analgesics, progressing to stronger options as needed. Nonsteroidal anti-inflammatory drugs (NSAIDs) may offer initial relief, but their long-term efficacy is often limited due to the neuropathic nature of CRPS pain.
Neuropathic pain medications, such as gabapentin – noted in treatment schemes from 2017 – and pregabalin, are frequently employed to modulate nerve pain signals. Tricyclic antidepressants (TCAs) and serotonin-norepinephrine reuptake inhibitors (SNRIs) can also be beneficial, impacting pain pathways and mood. In some cases, opioid analgesics may be considered, but their use is generally reserved for carefully selected patients due to potential risks and the development of tolerance.
Local anesthetic injections, including nerve blocks and sympathetic blocks, can provide temporary pain relief and aid in diagnosis. Corticosteroid injections, as part of basic schemes, may reduce inflammation. It’s crucial to remember that pharmacological interventions are most effective when integrated within a comprehensive treatment plan, including dedicated physical therapy protocols.
Psychological Support & Cognitive Behavioral Therapy (CBT)
The profound impact of chronic pain on mental well-being necessitates integrated psychological support for CRPS patients. CRPS frequently co-occurs with anxiety, depression, and post-traumatic stress, significantly influencing pain perception and functional capacity. Addressing these psychological factors is paramount for successful treatment outcomes, complementing physical therapy interventions.
Cognitive Behavioral Therapy (CBT) emerges as a cornerstone of psychological management. CBT equips patients with coping mechanisms to reframe negative thought patterns, manage pain-related fear and avoidance behaviors, and enhance self-efficacy. Techniques include relaxation training, activity pacing, and goal setting.
Furthermore, acceptance and commitment therapy (ACT) can assist patients in accepting pain as a part of their experience, focusing on living a meaningful life despite discomfort. Support groups provide a valuable platform for peer connection and shared experiences. A holistic approach, acknowledging the interplay between physical and psychological factors, is essential for optimizing CRPS management.
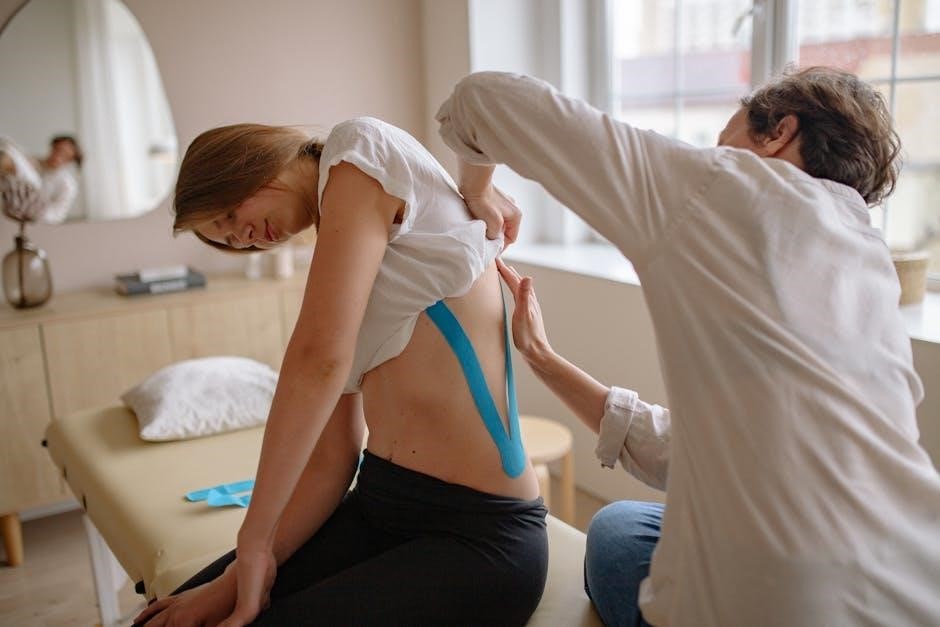
Long-Term Management & Prevention of Flare-Ups
Sustained benefit requires diligent adherence to a home exercise program, ongoing patient education, and proactive self-management strategies to minimize potential symptom exacerbations.
Home Exercise Program
A carefully designed home exercise program is paramount for long-term CRPS management, reinforcing gains achieved during formal physical therapy sessions. This program should be highly individualized, considering the patient’s specific limitations and pain levels, and progressively challenging as tolerated.
Initially, the focus remains on maintaining range of motion through gentle, pain-free movements performed several times daily. As pain subsides, exercises can gradually incorporate strengthening components, targeting affected limbs and surrounding musculature. Proprioceptive exercises, enhancing body awareness, are also crucial.
Patients must be educated on recognizing flare-up triggers and modifying activity accordingly. Consistent, low-impact activity is generally preferred over infrequent, strenuous bouts. Detailed written instructions, potentially supplemented with video demonstrations, are essential for proper execution and adherence. Regular communication with the physical therapist allows for program adjustments and addresses any emerging challenges, ensuring continued progress and preventing symptom recurrence.
Patient Education & Self-Management Strategies
Empowering patients with comprehensive knowledge about CRPS is fundamental to successful long-term management. Education should cover the condition’s pathophysiology, potential triggers, and the rationale behind the treatment plan, fostering a sense of control and reducing anxiety.
Self-management strategies include pacing activities to avoid overexertion, utilizing relaxation techniques like deep breathing or mindfulness to modulate pain, and recognizing early warning signs of flare-ups. Maintaining a pain diary can help identify patterns and triggers.
Patients should understand the importance of adhering to the home exercise program and communicating any changes in symptoms to their healthcare team. Psychological support, potentially through CBT, is vital for coping with the emotional impact of chronic pain. Active participation in their care, coupled with realistic expectations, significantly improves outcomes and quality of life.
